Intragastric balloons (IGBs) is becoming a minimally invasive, reversible option for weight management for the patients who are unable to achieve sufficient weight reduction through lifestyle modification alone. IGBs is between conservative medical therapy and bariatric surgery, which can provide a short-term intervention to achieve significant weight loss, at the same time, avoiding permanent anatomical changes.
Clinical Efficacy of IGB:
There's multiple randomized controlled trials and meta-analyses confirm that IGB therapy combined with structured lifestyle modification produces superior weight reduction compared with lifestyle modification alone. On average, patients can achieve 10–20% total body weight loss (TBWL) within 6–12 months of therapy. This kind of weight reduction is clinically meaningful, as it correlates with improvements in metabolic parameters such as glycemic control, blood pressure, and lipid profile. It's also important that the sustainability of weight loss depends largely on adherence to dietary and behavioral interventions after balloon removal, highlighting the need for multidisciplinary follow-up.
Device Types and Key Differences:
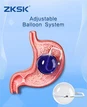
IGBs are broadly categorized into three groups: non-adjustable, adjustable, and procedure-less swallowable balloons.
- For non-adjustable balloons, it's placed and removed through endoscope, with a typical residence time of six months. They're the most widely studied and are supported by robust safety and efficacy data.
- For adjustable balloons, it allow intragastric volume modification during therapy. Clinical evidence shows that increasing balloon volume after a weight-loss plateau can stimulate further reduction, while deflation can improve tolerance in patients with intolerance symptoms. This individualized approach is advantageous but may be associated with higher technical complexity and a slightly increased risk of complications.
- And for procedure-less swallowable balloons, they are ingested in capsule form and can naturally excreted after approximately 16 weeks. This method eliminates the need for endoscopy and anesthesia, improving patient acceptance. Some short-term studies demonstrate promising efficacy and safety, though long-term outcomes are still under investigation.
Safety and Complications of IGB
IGBs are generally safe when placed in appropriately selected patients. The most common adverse events are transient nausea, vomiting, and abdominal discomfort during the first days placed. More serious complications, such as balloon deflation with migration, gastrointestinal obstruction, or perforation are rare but clinically significant. How to minimize the risks? by careful patient selection, adherence to manufacturer guidelines, and close clinical monitoring are essential to minimize risks.
Guideline Recommendations
Professional societies such as the American Gastroenterological Association (AGA) and the American Society for Metabolic and Bariatric Surgery (ASMBS) recommend IGBs for adults with a body mass index (BMI) of 30–40 kg/m², or as a bridge to bariatric surgery in higher-risk patients. They emphasize that IGB therapy should always be integrated into a structured weight management program involving dietary counseling, physical activity, and psychological support.
Future Directions
The next generation of IGBs is moving toward greater patient convenience, improved safety, and enhanced personalization:
- Longer-lasting devices with biodegradable materials are under development, potentially extending treatment duration without requiring endoscopic removal.
- Smart balloons with digital sensors could allow real-time monitoring of balloon position, pressure, and gastric environment, improving safety and facilitating remote follow-up.
- Combined therapy approaches are being studied, where IGBs are used alongside pharmacological agents (such as GLP-1 receptor agonists) to maximize efficacy.
- Patient-centered design is expected to reduce intolerance rates, with balloons that are easier to swallow, more comfortable, and adaptable to different patient profiles.
- Broader global accessibility may be achieved as swallowable, non-endoscopic balloons expand adoption in regions with limited endoscopy infrastructure.